Senior Investigator Research Interests
Branching morphogenesis is a fundamental attribute of many organ systems. The overarching goal of Dr. Mukouyama’s laboratory is to uncover the molecular control of the morphologic processes underlying the patterning of tubular branching networks, particularly the vascular and nervous systems, which share several anatomic and functional characteristics, and are often patterned similarly in peripheral tissues. These characteristics suggest that there is interdependence between these two networks during tissue development and homeostasis. Thus, Dr. Mukouyama is studying neuronal influences on vascular branching patterns and vascular influences on both neuronal guidance and neural stem cell maintenance. His laboratory approaches these problems using a combination of high-resolution whole-mount imaging, molecular manipulations, advanced genetic perturbations, next-generation sequencing, and in vitro organ culture techniques.
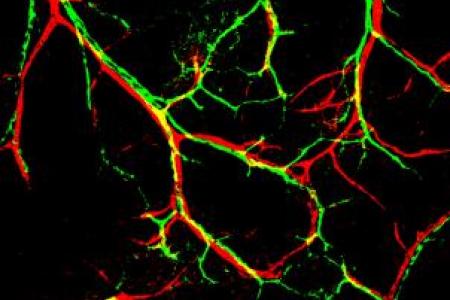
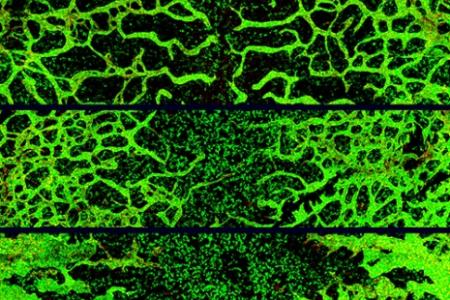
By developing a model system of skin vasculature that allows for the direct observation of congruent vascular and neural networks in an anatomically recognizable pattern, Dr. Mukouyama and his colleagues have begun to unravel the neural control of vascular development. Their work has established two distinct developmental mechanisms: nerve-derived VEGF-A controls arterial differentiation, and nerve-derived CXCL12 controls vessel branching and nerve alignment. With a combination of high-resolution whole-mount imaging in vivo Ca2+ indicator mice, they are currently examining what happens to sensory activity in the mutants having neuro-vascular mis-patterning in developmental and pathological situations, including obesity-related nerve disorders. These studies will provide novel conceptual advances in the development and maintenance of functional neurovascular wiring.
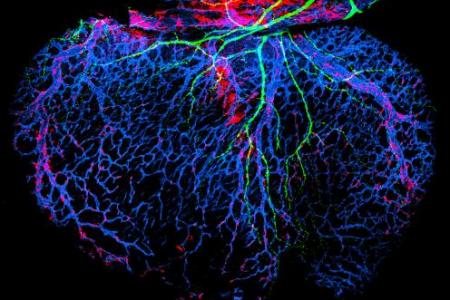
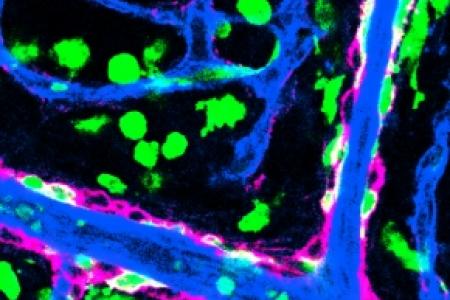
Just as nerves influence vascular patterns in the skin, Dr. Mukouyama and his colleagues have also shown that blood vessels influence nerve patterns in the developing heart. Using whole-mount imaging, they demonstrated that sympathetic axons branch alongside large-diameter coronary veins in the sub-epicardial layer of the dorsal ventricular wall prior to innervating final targets such as coronary arteries and cardiomyocytes in the deeper myocardial layer. This novel neuro-vascular association is established by sequential expression of NGF in the subepicardial venous vascular smooth muscle cells (VSMCs) and myocardial arterial VSMCs of coronary vessels. With an ultra-high-frequency non-invasive imaging, they found abnormal cardiac functions such as irregular cardiac rhythms in the mutant embryos lacking autonomic nervous system. They are currently examining what happens to the myocardium development and conduction system architecture in the absence of autonomic nervous system and how autonomic nerves affect cardiomyocyte differentiation and maturation. These studies will provide a mechanistic framework for the functional consequence of sympathetic innervation in the developing heart.
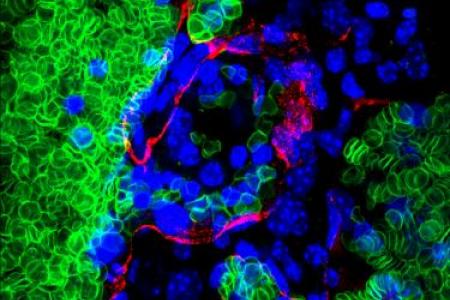
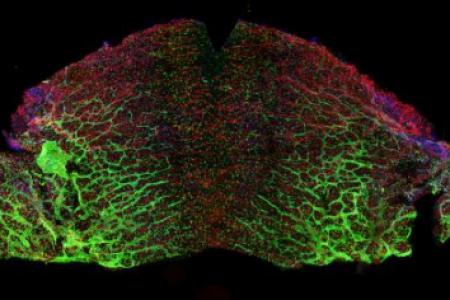
No examination of neurovascular interactions could neglect the brain. The vasculature component of this specialized niche microenvironment helps to retain neural stem cell potential. Dr. Mukouyama and his colleagues have also found that brain vasculature influences unique distributions of embryonic macrophages including parenchymal microglia, as well as non-parenchymal meningeal and perivascular macrophages. They are currently examining how embryonic macrophages regulate radial glial cells, the primary source of cortical neurons in early brain development. These studies will provide insights into understanding the molecular and cellular basis of the neuro-vascular-immune interactions in the developing brain.
These three independent but thematically interrelated projects provide unique opportunities to advance understanding of the dynamic features of both vascular and neuronal branching networks.
Meet the Team

Yosuke Mukoyama, Ph.D.
Yoh-suke Mukouyama, whose legal name is Yosuke Mukoyama, publishes as Yoh-suke Mukouyama. He received his A.B. in pharmacy studies from Tokyo University of Science and his M.S. and Ph.D. in developmental biology from the University of Tokyo. As a student in the laboratory of Atsushi Miyajima, he studied the properties of embryonic endothelial cells and hematopoietic stem cells (HSCs). He did postdoctoral research in the laboratory of David Anderson at the California Institute of Technology where he demonstrated that peripheral nerves direct arterial organization and formation by secreting VEGF; he also studied the properties of neural stem cells (NSCs). Dr. Mukouyama joined the NHLBI as a tenure-track Investigator in 2006. He also serves on the editorial board of Developmental Dynamics and is a member of the International Society for Stem Cell Research and the North American Vascular Biology Organization.
Contact the lab

Krista Gill, B.S.

Wenling Li, Ph.D.

William Kowalski, Ph.D.

Yuta Koui, Ph.D.

Ryo Sato, M.D., Ph.D.

Sara Gonzalez, PhD

Shuxuan Song

Join Our Lab
There are no current openings.
Please check back soon.